RESOURCES
OBJECTIVES & QUESTIONS
Summary
What are the functions of the pancreas?
Exocrine Functions
- Alkaline secretion to buffer gastric pH:
- Protects duodenal mucosa
- Produces optimal pH range for pancreatic enzymes
- Enzymatic digestion (Trypsin, Amylase, Elastase, Lipase)
Endocrine Functions
- Secretion of hormones to regulate blood sugar (Insulin, Glucagon, Somatostatin)
Which structures in the pancreas are dedicated to the endocrine and exocrine functions?
Microscopically divided in to exocrine and endocrine cells:
Exocrine Cells
- Vast majority of pancreatic tissue (99%)
- Acinar and ductal cells secrete alkaline digestive secretions containing enzymes
- Drain via pancreatic ductules and ducts which unite with the common bile duct opening in to the duodenum
Endocrine Cells
- Occupy on 1% of the pancreatic tissue
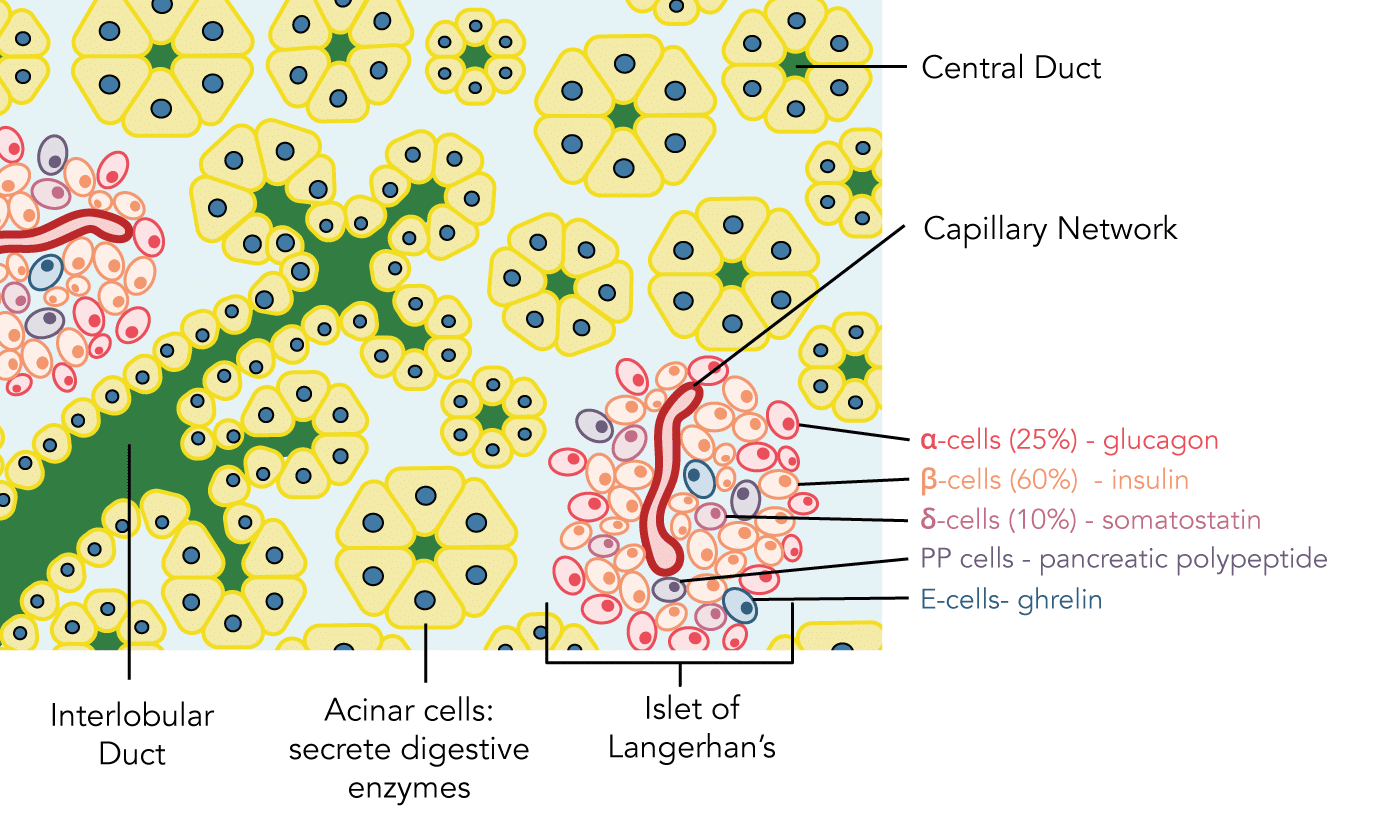
- Located in collections called the "islets of Langerhans":
- Approximately 1 million scattered throughout acinar cells
- Possess different cell types which produce, store and secrete different hormones:
- α-cells (25%) - glucagon
- β-cells (60%) - insulin
- δ-cells (10%) - somatostatin
- PP cells - pancreatic polypeptide
- E-cells - ghrelin
Overview of Exocrine Function
Where do pancreatic exocrine secretions originate from and how much is created daily?
- A total of 1.5 L of pancreatic juice is produced per day
- Drains into the duodenum through the pancreatic duct.
- The main cells of the exocrine pancreas are:
- Acinar cells – produce digestive enzymes
- Ductal cells – secrete HCO3 ̅ and water
Which digestive enzymes are produced by the pancreas and what are their functions?
Protein Breakdown
Protein Breakdown
- Trypsinogen
- Chymotrypsinogen
- Elastase
- Endopeptidases - cleave bonds between amino acids
- Split whole and partially digested proteins into peptides of various sizes but do not cause release of individual amino acids.
- Carboxypeptidase
- Aminopeptidase
- Exopeptidases - cleave bonds at the terminus of a peptide
- Splits peptides into individual amino acids, thus completing digestion of some proteins to amino acids.
Carbohydrate Breakdown
Carbohydrate Breakdown
- α-amylase
- Hydrolyses carbohydrates (starch and glycogen) to form mostly disaccharides and a few tri-saccharides.
- Has no activity against cellulose
Lipid Breakdown
Lipid Breakdown
- Pancreatic lipase
- Phospholipase
- Hydrolyses triglycerides and subsequently into monoglycerides and free fatty acids
What protects pancreatic tissue from digestive enzymes?
- Pancreatic enzymes are secreted in inactive form
- The suffix –ogen or prefix pro- indicates an inactive enzyme (e.g. trypsinogen, procarboxypeptidase
- They will be activated by:
- Enterokinase enzyme: secreted by the brush border of the duodenal wall when chyme comes into contact
- Autocleavage: by previously activated trypsin which can subsequently activate trypsinogen, chymotrypsinogen and procarboxypeptidase
- Acinar cells also secrete the enzyme trypsin inhibitor:
- Prevents activation of trypsin inside acini and ducts
- Protective ability can become overwhelmed if duct becomes blocked leading to autodigestion and acute pancreatitis
Regulation of Exocrine Function
How are pancreatic secretions controlled?
- Minimal secretion between meals
- Entry of food stimulates secretions via neural and humoral mechanisms:
Neural
- Pancreas is innervated by the vagus nerve which releases acetyl choline
- When activated during the cephalic phase of digestion in anticipation of a meal, there is an increase in pancreatic acinar cell activity
Humoral (Hormonal)
Gastrin
- Secreted by the G cells of the stomach in response to gastric distension
- Functions include:
- Stimulation of pancreatic acinar cells to secrete digestive enzymes in preparation for the arrival of carbohydrates, proteins and fats
- Stimulation of gas gastric acid secretion by the parietal cells of the stomach
Cholecystokinin (CCK)
- Secreted by the duodenal mucosal cells in response to fat or protein rich chyme entering the duodenum
- Functions include:
- Increasing the production of bile in the liver
- Stimulation of gallbladder contraction
- Slowing gastric emptying
- Stimulation of the pancreatic acinar cells to secrete digestive enzymes
Secretin
- Secreted by the duodenal mucosa in response to the presence of acid-containing chyme in the duodenum
- Functions include:
- Slowing gastric emptying
- Stimulation of duct cells of the pancreas to secrete HCO ̅ to neutralise chyme
What are the phases involved in pancreatic exocrine secretions?
1. Cephalic Phase
- Describes the activity that occurs in anticipation of a meal
- Signals are transmitted from the brain via the vagus nerve causing release of acetylcholine in nerve endings in the pancreas
- Causes moderate amounts of enzymes to be secreted into the pancreatic acini, accounting for about 20 percent of the total secretion after a meal
- Only small amounts of water is secreted which limits flow of enzymes through ducts at this stage
2. Gastric Phase
- Continues neural stimulation of enzyme secretion continues, accounting for another 5 to 10 percent of pancreatic enzymes secreted after a meal
- Fluid secretion again remains small, limiting amount that reaches the duodenum
3. Intestinal Phase
- As chyme enters the small intestines the pancreatic secretions become copious
- Mainly in response to the hormone secretin
Overview of Endocrine Function
Which hormones are secreted by the endocrine pancreas and what are their functions?
Hormone
Production
Function
Insulin
Beta (ß) cells
- Acts to decrease plasma glucose levels (hypoglycaemic hormone)
- Promotes uptake especially into liver, muscles, and adipose tissue.
Glucagon
Alpha (α) cells
- Acts to increase plasma glucose levels (hyperglycaemic hormone)
- Promote hepatic glycogenolysis and gluconeogenesis
Somatostatin
Delta (δ) cells
- Inhibits the secretion of multiple hormones
- These include: growth hormone, insulin, glucagon, gastrin, vasoactive intestinal peptide (VIP), and thyroid-stimulating hormone
Ghrelin
Epsilon (E) cells
- Suppresses insulin via paracrine interaction with beta cells
- Stimulates appetite
- Stimulates growth hormone secretion
Amylin
Beta (ß) cells - co-secreted with insulin
- Suppresses glucagon via paracrine interaction with alpha cells
- Slows gastric emptying which delays absorption of glucose from the small intestine into the circulation
- Stimulates the satiety centre of the brain
Pancreatic Polypeptide
PP cells -previously upsilon (F) cells
- Function unknown
- Primarily used as marker for other pancreatic endocrine tumours
Pancreatic Hormones
Describe the structure, secretion, function and regulation of insulin?
Insulin
Structure, Sythesis & Transport
- A peptide hormone made of 51 amino acids
- Formed of 2 chains (α and β) connected by disulphide bridges
- Synthesised as proinsulin with chains joined by C-peptide
- C-peptide excised by endopeptidases in the endoplasmic reticulum of β cells prior to release
- C-peptide is 31 amino acid sequence has no known biological function
- Can be used as marker of endogenous insulin secretion
- Stored in secretory granules and is secreted by the cells via exocytosis
- It enters the portal system with half cleared by first pass through the liver
- Circulates entirely in an unbound form
Function
- Key to glucose homeostasis - 'hypoglycaemic anabolic hormone':
- Liver:
- Promotes glycolysis and storage of glucose as glycogen (glycogenesis)
- Promotes conversion of glucose to triglycerides
- Muscle
- Promotes the uptake of glucose and its storage as glycogen
- Adipose tissue:
- Promotes uptake of glucose and its conversion to triglycerides for storage.
Mechanism of Action
- Binds to a specific receptor tyrosine kinase on the plasma membrane
- Increases its activity to of numerous numerous regulatory enzymes and promotes glucose transport in to cells by increasing membrane permeability
Regulation
Stimulated by:
- Raised plasma glucose
- Raised plasma fatty acid & ketone bodies
- Vagal nerve stimulation
- Amino acids
- Gut hormones (gastrin, secretin, CCK, and GIP)
Inhibited by:
- Sympathetic stimulation
- Somatostatin
Describe the structure, secretion, function and regulation of glucagon?
Glucagon
Structure, Sythesis & Transport
- A peptide hormone made of 29 amino acids
- Formed as a prohormone named pro-glucagon and cleaved to glucagon
Function
- Key to glucose homeostasis - 'hyperglycaemic catabolic hormone':
- Actions virtually all in the Liver:
- Promotes glycogenolysis - low levels
- Promotes gluconeogenesis - medium levels
- Promotes lipolysis, fatty acid oxidation, and ketogenesis - high levels
- Acts synergistically with catecholamines, glucocorticoids, and growth hormone
Mechanism of Action
- Binds to a specific G protein coupled receptor on the plasma membrane stimulating adenylyl cyclase
- Results in the phosphorylation and activation of numerous regulatory enzymes and other protein substrates
Regulation
Stimulated by:
- Low plasma glucose
- Sympathetic stimulation
Inhibited by:
- Raised plasma glucose
- Somatostatin
- Raised plasma fatty acid & ketone bodies

